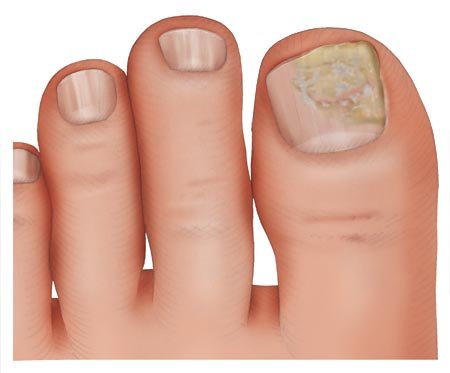
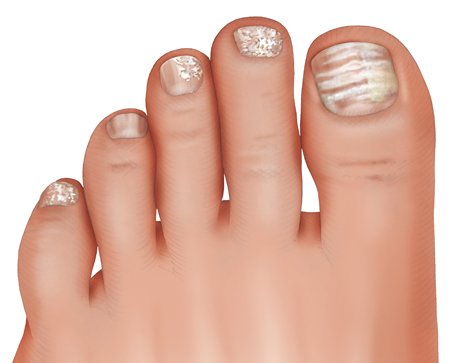
De Berker D. Clinical practice. Fungal nail disease. N Engl J Med 2009; 360(20): 2108-2116.
Deutsche Dermatologische Gesellschaft (DDG), Deutschsprachige Mykologische Gesellschaft (DMykG). Tinea der freien Haut (S1-Leitlinie, in Überarbeitung). AWMF-Registernr.: 013-002. 2008. http://www.oegstd.at/res/013-002.pdf
Eisman S, Sinclair R. Fungal nail infection: diagnosis and management. BMJ 2014; 348: g1800.
Gupta AK, Daigle D, Foley KA. Network Meta-Analysis of Onychomycosis Treatments. Skin Appendage Disord 2015; 1(2): 74-81.
Gupta AK, Daigle D, Foley KA. Topical therapy for toenail onychomycosis: an evidence-based review. Am J Clin Dermatol 2014; 15(6): 489-502.
Kreijkamp-Kaspers S, Hawke K, Guo L et al. Oral antifungal medication for toenail onychomycosis. Cochrane Database Syst Rev 2017; (7): CD010031.
Matricciani L, Talbot K, Jones S. Safety and efficacy of tinea pedis and onychomycosis treatment in people with diabetes: a systematic review. J Foot Ankle Res 2011; 4: 26.
IQWiG health information is written with the aim of helping people understand the advantages and disadvantages of the main treatment options and health care services.
Because IQWiG is a German institute, some of the information provided here is specific to the German health care system. The suitability of any of the described options in an individual case can be determined by talking to a doctor. informedhealth.org can provide support for talks with doctors and other medical professionals, but cannot replace them. We do not offer individual consultations.
Our information is based on the results of good-quality studies. It is written by a team of health care professionals, scientists and editors, and reviewed by external experts. You can find a detailed description of how our health information is produced and updated in our methods.