How is paroxysmal supraventricular tachycardia (PSVT) treated?

If your heart sometimes suddenly beats very fast, you may have paroxysmal supraventricular tachycardia (PSVT). This abnormally fast heart rate can often be slowed down with certain breathing techniques and body positions (Valsalva maneuver) or with medication. A catheter procedure can prevent episodes in the long term.
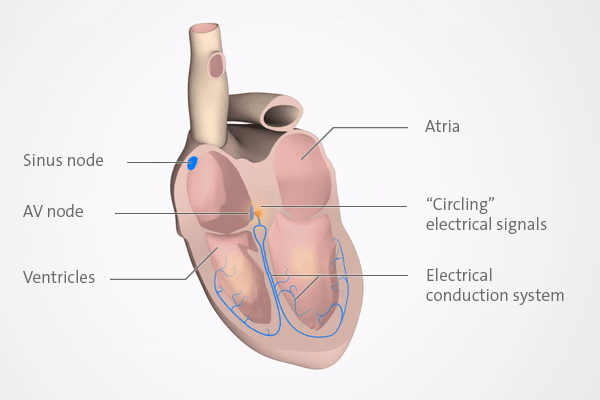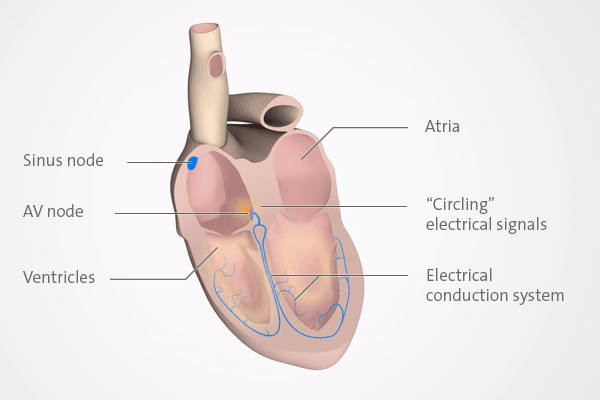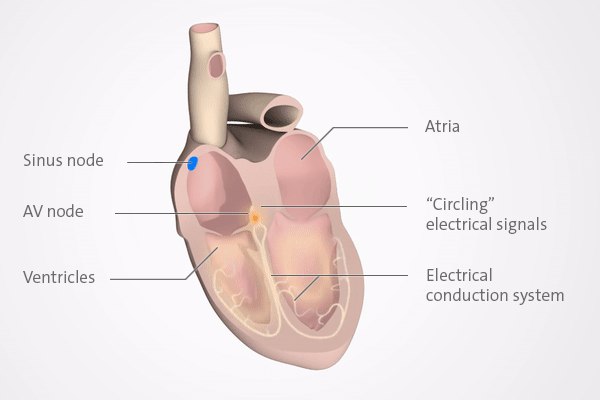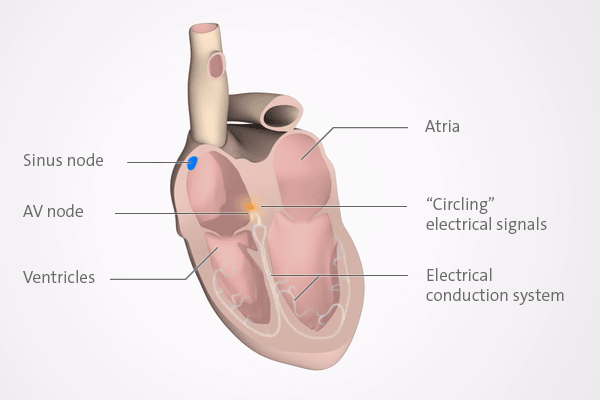
PSVT is a relatively common but generally harmless heart rhythm disorder (arrhythmia). It makes the heart beat very fast (tachycardia) for several minutes or, in rare cases, for more than an hour. The racing heart in PSVT is usually caused by a problem in an area of the heart known as the AV node.
The fast heart rate usually stops just as suddenly as it started. During an episode, it can be felt as palpitations (pounding or fluttering) in the chest. That may be accompanied by symptoms like dizziness, shortness of breath or chest pain. In rare cases, people might faint and fall. Serious complications like ventricular fibrillation are rare too. The risk is greater if the fast heart rate is caused by extra electrical pathways in the heart that were there at birth (congenital).