Introduction
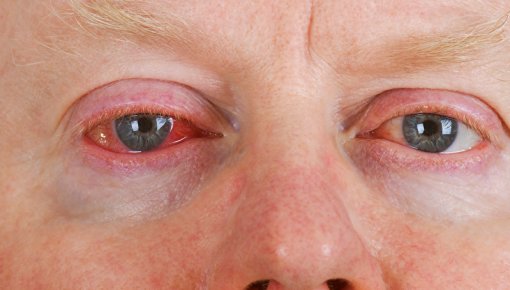
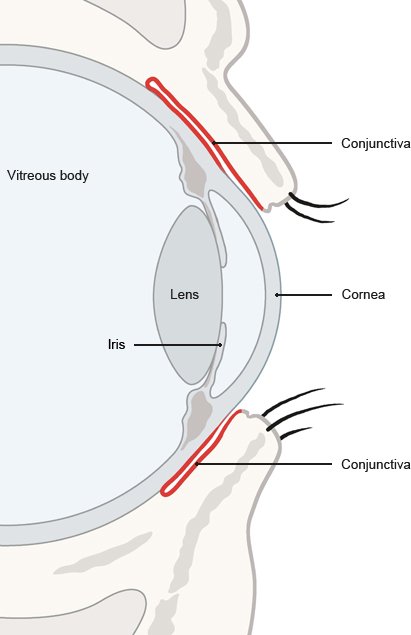
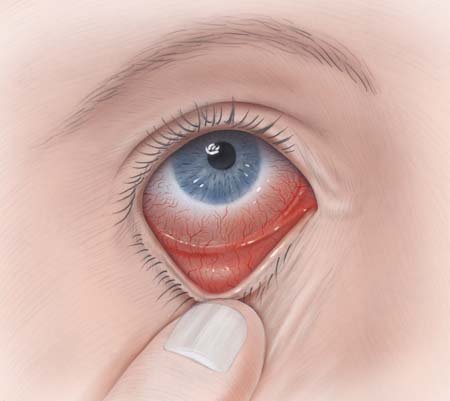
Conjunctivitis, also known as pink eye, is an inflammation of the conjunctiva. This is a protective membrane that covers the visible white part of the eye and the inner side of the eyelid. Conjunctivitis makes the affected eye(s) turn red.
The inflammation is commonly caused by germs such as viruses or bacteria (infectious conjunctivitis). But it is also often caused by an allergy (allergic conjunctivitis).
It often affects both eyes because the infection can easily spread from one eye to the other. To prevent this from happening, it’s important to avoid touching an infected eye. If you do touch it, be sure to wash your hands right away. It is also a good idea to use your own towels and washcloths, and not share them with other people.