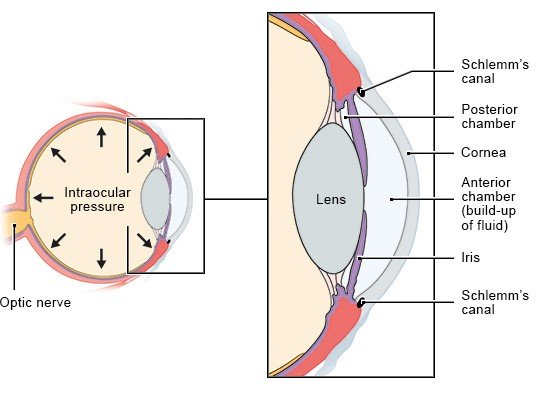
Many people who are found to have high intraocular pressure will feel quite nervous about it, even though their vision is still perfectly fine. Just knowing that you have high intraocular pressure, and therefore a higher risk of developing glaucoma, may cause you to worry about even the slightest trouble with your vision, although it may have nothing to do with glaucoma.
People with glaucoma are often very scared of going blind. Especially at the start, many people want to find out all about the treatment and how the diagnosis might affect their life.
If glaucoma leads to major vision loss, everyday life needs to be adjusted to the new situation. Things at home can be set up to make it easier to find your way around – for instance, by adding additional sources of light. Removing tripping hazards is important too, in order to prevent falls. It is also usually possible to make changes at work or in everyday activities such as sports, shopping or reading. Seeking support and finding out about things that could help you – for instance, by asking your doctor or health insurer – can make everyday life easier. Many people who have glaucoma also find it helpful to find out more about the condition and ways to cope with its effects, or to talk with other people who have glaucoma – for instance, in a support group or on an internet forum.
It is often difficult to recognize the point at which glaucoma makes it impossible to drive a car safely. At first, people with glaucoma often start making changes to their driving habits, for instance by no longer driving at night or only sticking to familiar streets. It is important to try to be aware of when your vision becomes too much of a problem and you start putting yourself and others at risk. Once a certain amount of eyesight has been lost, driving is illegal. Your eye doctor can give you more specific information and advice.
It is not easy to deal with worsening vision and being increasingly dependent on other people. But you may eventually have to give up control in some areas of your life. Other people can then help you to keep up your usual activities as much as possible and to maintain social contacts.
Talking about your worries and fears with family and friends early on can be a great relief. Together you can develop strategies for dealing with worsening eyesight. Having people who are there for you and who understand and support you can really make things easier in life – particularly if you’re dealing with a difficult health problem and want to stay as active as you can.