Benefits and risks of screening tests
A wide range of screening tests are available. Some tests are considered to have a benefit, whereas the benefit of other tests is not so clear. We describe which criteria a screening test must fulfill for it to be worth having, explain important terms, and shed light on the scientific background.
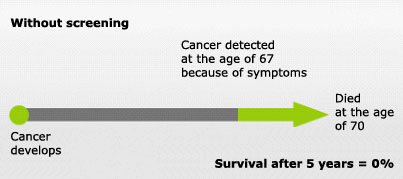
Diagnostic tests are usually done to find out what is causing certain symptoms. Screening tests are different: they are done in people who do not feel ill. They aim to detect diseases at an early stage, before any symptoms become noticeable. This has the advantage of being able to treat the disease much earlier. However, treating a disease at an early stage only makes sense if it leads to a better health outcome than treating it at a later stage.
There are many different kinds of screening. For example, if all newborns are offered the same tests (like hearing tests), that is one kind of screening.
Another kind of screening is called opportunistic screening: this is where someone visits a doctor for a particular reason and, while they are there, they are offered an additional test, such as blood pressure measurement. In population-wide screening, everyone who fulfills the criteria for the test is invited to have a voluntary test. One example of this kind of screening in Germany is an x-ray examination of the breast (mammography) in women between the ages of 50 and 69, to screen for breast cancer.
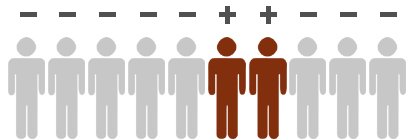
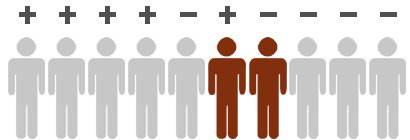
The medical tests used for screening purposes are often not suitable for making a final diagnosis. Instead, many tests are used to detect any abnormalities first, which are then looked at more closely in other tests. This is the case for stool tests done in bowel cancer screening, for example. The stool tests look for occult (hidden) blood in a person’s stool, which could be a sign of bowel cancer. If the test results are abnormal, the bowel is examined closely with an endoscope. This is the only way to find out whether the traces of blood are indeed being caused by cancer, or by a non-cancerous condition such as hemorrhoids or an inflammation of the lining of the bowel.
Screening tests are not always done to look for a disease. Some screening tests aim to detect risk factors for certain diseases. In Germany, members of statutory health insurance funds who are aged 35 and over are entitled to a general check-up called the “Gesundheits-Check-up,” for example. This includes a blood and urine test, as well as other things. The findings are not always clear. They sometimes lie in a gray area between normal and abnormal results.