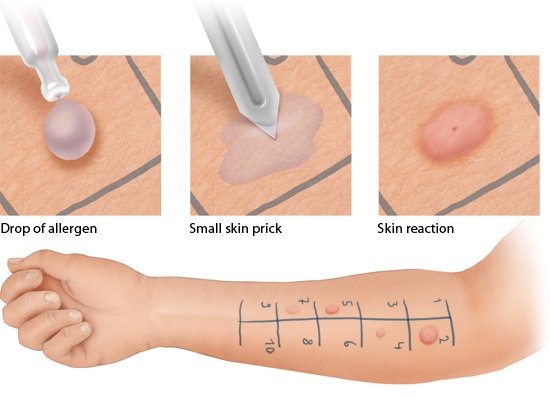
What kinds of allergy tests are there?
Allergies occur when the human immune system starts fighting substances that are in fact quite harmless, like pollen, dust or foods. The more sensitive the immune system is to a particular substance that triggers an allergic reaction (allergen), the more severe the resulting symptoms are. Allergies may cause watery or red eyes, sneezing attacks, a stuffy nose, an itchy rash or stomach ache. In rare cases an allergy may lead to an anaphylactic shock. Then the airways become narrow, making it very hard to breathe, and there is a severe drop in blood pressure. Anaphylactic shock can become life-threatening if not treated immediately.
Various tests can be used to find out what kind of substance is causing an allergic reaction: skin tests, blood tests and provocation tests. Your doctor will usually decide which test to use based on your description of the symptoms and your medical history.