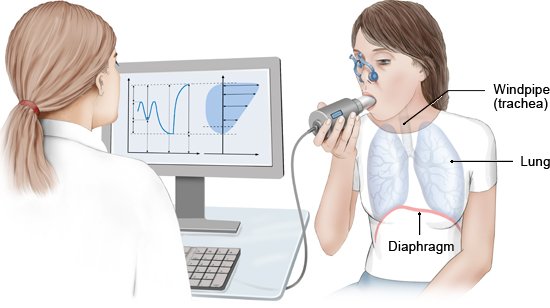
When are lung function tests needed?
It can be a good idea to have your lungs tested:
- if you have shortness of breath, a persistent cough, abnormal breathing sounds, or if you cough up phlegm,
- if an x-ray of your lungs shows abnormalities, or
- in order to prepare for surgery.
These tests are also used if doctors think you might have one of the following:
- Asthma
- Chronic obstructive pulmonary disease (COPD)
- Pulmonary fibrosis (lung tissue scarring)
- Pulmonary emphysema
And they can be used to monitor the treatment outcomes and the course of chronic lung diseases like asthma or COPD. They are sometimes part of employee health check-ups too, or used in sports medicine.