Introduction

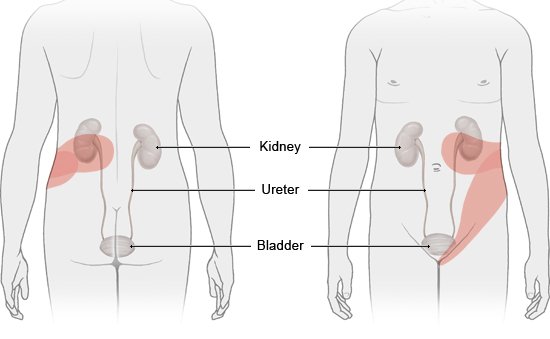
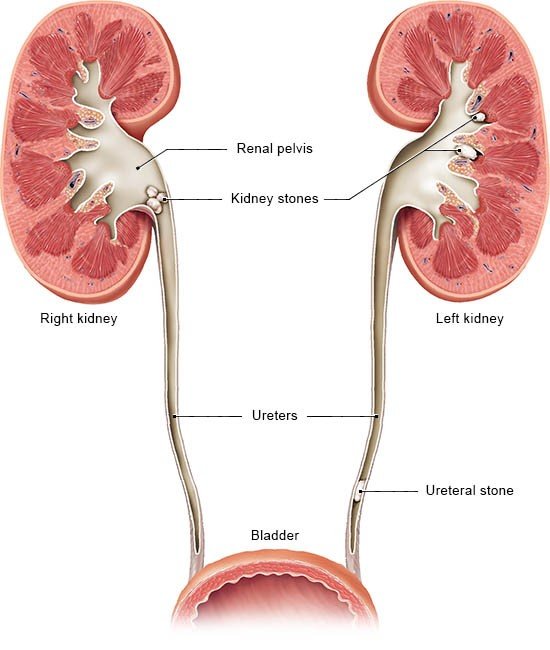
Kidney stones are small, hard deposits that can form in a part of the kidney called the renal pelvis. Those that enter a ureter are sometimes referred to as ureteral stones. The ureters are the tubes that carry urine from the kidneys to the bladder.
Many of these stones are so small that they are able to travel to the bladder in just a few days or weeks without any treatment, and then exit the body in your urine. If smaller stones are causing problems, it's often enough to take painkillers, drink plenty of fluids, move enough and simply wait for the kidney stones to pass through. Muscle-relaxing medications can be used to help pass medium-sized stones.
Larger stones may get stuck as they exit the renal pelvis or take longer to move through the ureter, causing severe pain and other symptoms. Then they usually need to be broken up by sound waves or removed through a minor surgical procedure. The most suitable treatment will depend on the size, type and position of the stones in the kidney or the urinary tract.
It is common to have kidney stones multiple times. Finding the cause is a necessary part of preventing that from happening.