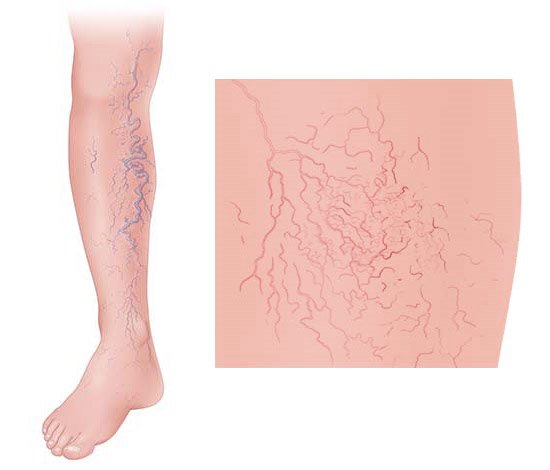
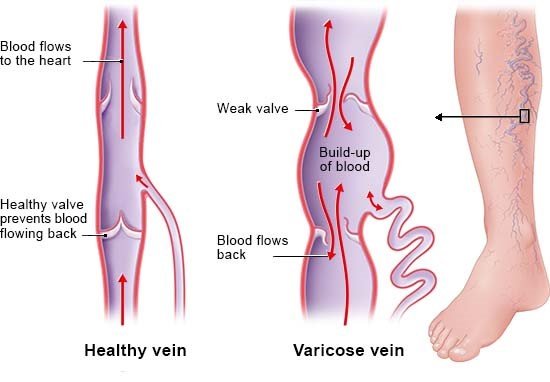
The following things are often recommended for the relief of varicose vein symptoms:
- Avoid standing or sitting for a long time
- Move as much as you can in everyday life
- Put up your legs when you sit
- Don't cross your legs when you sit
- Lose some weight if you are overweight
Compression stockings put pressure on the veins and are designed to support the flow of blood. But it’s not clear whether or how well they can help to reduce the symptoms of varicose veins. The same is true for weight loss.
There is also no proof of the effectiveness of creams, lotions, tablets or dietary supplements that are available for the treatment of vein problems. These products often contain horse chestnut or red vine leaf extracts.
If the symptoms of varicose veins are too severe or the veins are very distressing because of their appearance, then a medical procedure may help. Varicose veins can be surgically removed, sealed using heat or destroyed using chemicals.
These are the most common surgical procedures:
- Vein stripping: Two cuts (incisions) are made on the leg and the entire vein is pulled out through a cut near the groin.
- Phlebectomy: Several small cuts (just a few millimeters wide) are made along the affected vein, which is then removed in several pieces. This technique is mainly used to treat smaller veins.
Nowadays, varicose veins are often sealed off using heat because that is less likely to cause complications than surgery is. They can be sealed off in two ways:
- Radiofrequency ablation: A thin tube ( catheter) is inserted into the vein through a small cut. Then a transducer is guided into the catheter. The transducer sends out electromagnetic waves (radio waves). These waves produce heat that is used to seal off the veins.
- Endovenous laser ablation: This treatment also involves heating the vein from the inside to close it off, but lasers are used instead of radio waves.
Another treatment option is known as sclerotherapy. This approach involves injecting a liquid or foam into the affected vein. The drug that it contains damages the vein so much that it is transformed into connective tissue, sealing off the vein. One possible side effect of this treatment is the skin turning a brownish color at the injection sites. That usually goes away within a few weeks or months.
In Germany, not every health insurer will cover all of these treatments, so it's a good idea to find out in advance about which of them are covered.