Introduction

Digestive problems like nausea, belly ache or diarrhea can be caused by various things. One of them is celiac disease, sometimes called gluten-sensitive enteropathy or celiac sprue in the past. People with this condition have an abnormal reaction to gluten, which is a protein found in many cereals. Celiac disease (also spelt "coeliac") can develop at any age and does not go away. It can be treated effectively by following a strict gluten-free diet.
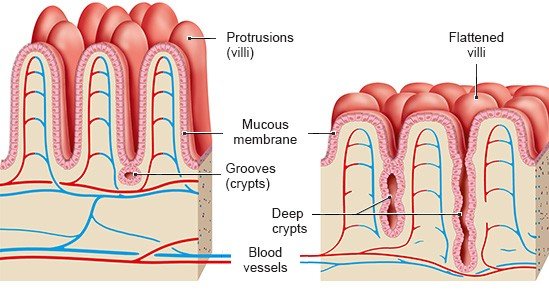
In celiac disease, the body’s immune system overreacts to parts of gluten that are usually harmless. Even the smallest amounts of gluten can then cause an inflammation in the soft lining (mucous membrane) of the small intestine. The immune system starts to attack the mucous membrane too, making the inflammation worse. This is referred to as an autoimmune reaction because the immune system attacks its own body. This reaction is the difference between celiac disease and a wheat allergy or wheat sensitivity.
If people with celiac disease continue to eat foods with gluten in them, they will end up with chronic inflammation in their small intestine. The mucous membrane lining the intestine changes and various symptoms may occur – not only in the digestive system.
Removing gluten from your diet makes the inflammation go down and the mucous membrane usually recovers. The symptoms then get better or disappear completely. Because a lot of foods contain cereals, it is especially important that people with celiac disease check food labels for traces of gluten.