Introduction

Diabetes is a metabolic disease that affects many parts of the body. Depending on the type of diabetes, the body either can't produce insulin itself (type 1) or it is unable to properly use the insulin it produces (type 2). Insulin is a hormone – a chemical messenger that is transported in the blood and regulates important body functions. Without insulin, your body can't get the energy it needs from the food you have eaten.
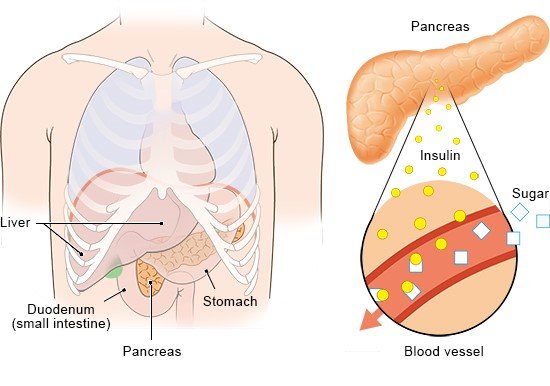
This vital hormone is usually produced in the pancreas and released into the bloodstream. It enables the sugar (glucose) in our food and drink to be transported into our cells and converted into energy for our bodies. Without insulin, our bodies can't use the sugar in our blood, so the sugar builds up there. Very high blood sugar concentrations cause a number of symptoms.
People with type 1 diabetes have to inject insulin every day because their pancreas can only produce very little insulin, or none at all. Insulin therapy helps to prevent strong fluctuations in blood sugar levels and the unpleasant short-term effects of high and low blood sugar. Another aim is to prevent health problems that may develop over time as a result of high blood sugar levels.