Dalal A, Eskin-Schwartz M, Mimouni D et al. Interventions for the prevention of recurrent erysipelas and cellulitis. Cochrane Database Syst Rev 2017; (6): CD009758.
Deutsche Dermatologische Gesellschaft (DDG), Deutsche Gesellschaft für Wundheilung und Wundbehandlung (DGfW), Deutsche Gesellschaft für Lymphologie (DGL) et al. S1-Leitlinie Differentialdiagnose akuter und chronischer Rötungen im Bereich der Unterschenkel. AWMF-Registernr.: 013-100. 2021.
Holm N, Burgdorf WH. Hauterkrankungen bei dunkelpigmentierten Menschen. In: Plewig G, Degitz K (Ed). Fortschritte der praktischen Dermatologie und Venerologie, vol 17. Berlin: Springer; 2001.
Kilburn SA, Featherstone P, Higgins B et al. Interventions for cellulitis and erysipelas. Cochrane Database Syst Rev 2010; (6): CD004299.
Moll I. Duale Reihe Dermatologie. Stuttgart: Thieme; 2016.
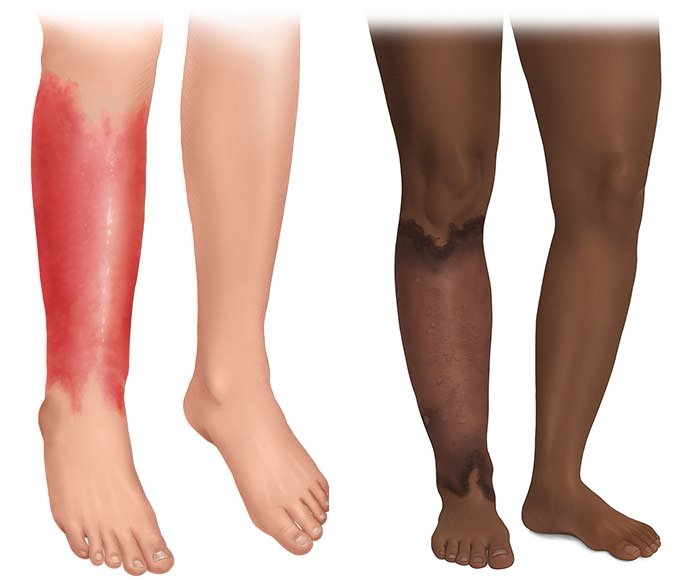
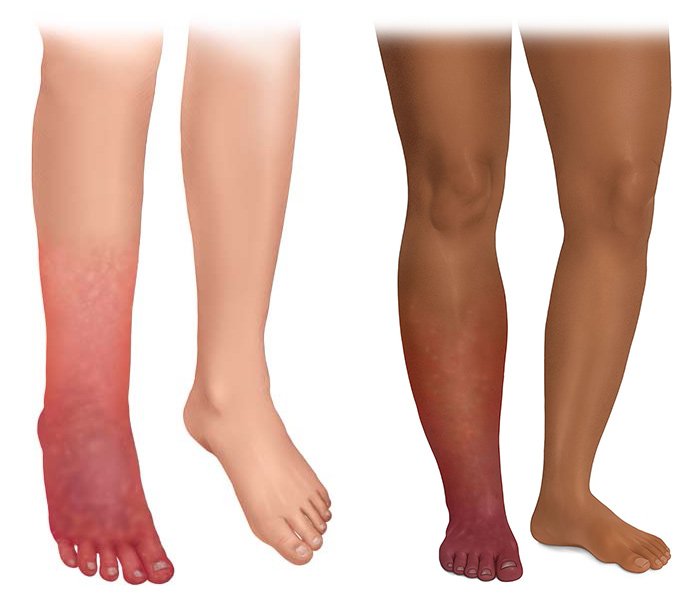
Mukwende M, Tamony O, Turner M. Mind the gap: A handbook of clinical signs in black and brown skin. London: St George's University; 2020.
Oh CC. Cellulitis and erysipelas: prevention. BMJ Clin Evid 2015: pii: 1708.
Oh CC, Ko HC, Lee HY et al. Antibiotic prophylaxis for preventing recurrent cellulitis: a systematic review and meta-analysis. J Infect 2014; 69(1): 26-34.
Phoenix G, Das S, Joshi M. Diagnosis and management of cellulitis. BMJ 2012; 345: e4955.
Quirke M, Ayoub F, McCabe A et al. Risk factors for nonpurulent leg cellulitis: a systematic review and meta-analysis. Br J Dermatol 2017; 177(2): 382-394.
Stevens DL, Bisno AL, Chambers HF et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis 2014; 59(2): e10-52.
Stevens DL, Bryant AE. Impetigo, Erysipelas and Cellulitis. National Center for Biotechnology Information (National Library of Medicine; NIH) 2016.
IQWiG health information is written with the aim of helping people understand the advantages and disadvantages of the main treatment options and health care services.
Because IQWiG is a German institute, some of the information provided here is specific to the German health care system. The suitability of any of the described options in an individual case can be determined by talking to a doctor. informedhealth.org can provide support for talks with doctors and other medical professionals, but cannot replace them. We do not offer individual consultations.
Our information is based on the results of good-quality studies. It is written by a team of health care professionals, scientists and editors, and reviewed by external experts. You can find a detailed description of how our health information is produced and updated in our methods.