There are various reasons for needing an eye examination, for instance sudden vision problems, other eye trouble or an injury. Regular check-ups are also important for keeping your eyes healthy if you have a higher level of risk for eye diseases. But what can you expect when you go in to see an eye doctor?
What do general eye examinations involve?
Eye examinations all usually tend to be quite similar. First you can talk about any sorts of problems you are having, like pain or poor vision. The doctor will first ask you about
- how long you have had these problems,
- whether they started suddenly or gradually, and
- whether both eyes are affected, or just one.
If you are in pain, it is important to describe as best you can where your eye hurts – e.g. on the surface, inside the eye or only when you move it? Does the pain spread out towards your forehead or temple?
Other information about your eyes is important too: Do you wear glasses or contact lenses? Have you already been diagnosed with an eye disease or are there other medical conditions that may be affecting your eyes, like diabetes? Your doctor will also ask whether you have any close relatives with glaucoma.
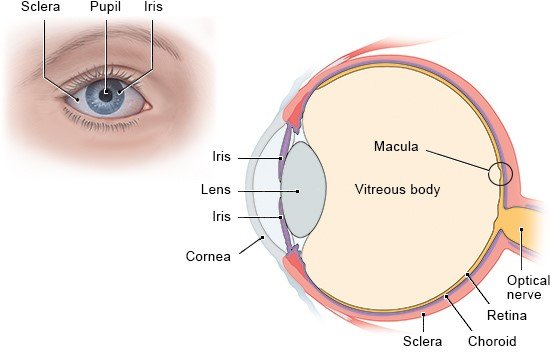
You will be checked for any irregularities, like an inflamed liver, injuries or visible differences between your two eyes. And the doctor will look to see whether your conjunctiva (the membranes lining the visible part of the eyeball and the inner surface of the eyelids) are reddened or inflamed. After that, the vision in each eye is tested using various instruments. The doctor uses a slit lamp to look at the front part of your eye under high magnification. An additional magnifying lens can be used to look inside the eye. They will also measure the pressure inside the eyeball – which is called intraocular pressure. Sometimes, more examinations are needed, depending on your symptoms and any medical conditions that you already have.
How is visual acuity measured?
A vision test measures your visual acuity, which is how far two points need to be apart from each other for you to actually perceive them as two separate points. The closer together the points are and the further away they are from you, the more difficult this becomes.
One of your eyes is covered for the test. With the other eye, you look at a chart or screen with letters, numbers or symbols of decreasing size.
Your visual acuity is measured by determining which of the figures you can still recognize from five meters away (about 16.5 feet). Sometimes the eye doctor will also check your visual acuity by having you read from a card with a similar chart on it at a distance of about 30 centimeters (12 inches). You repeat the tests with your glasses or contacts, if you have them.
It is not possible to do this test with very young children or people who have trouble communicating. There are other tests that can be used to get an approximate measure of their vision.
How is refraction measured?
Your eye’s refraction is tested to find out whether you need glasses, and if so, the strength of your prescription. The refraction is measured using special instruments. When you look through a device called a phoropter, it detects how your eye reflects the what you see and can calculate the refraction.
Another option involves a special instrument called a retinoscope. The doctor uses the retinoscope to move a beam of light across your pupil. Then lenses of varying strengths are held over your eye to see how the ray of light moves in your eye.
After that, another vision test is done: You again take a look at an eye chart or an image, but this time using different strengths of corrective lenses. Then you let the doctor know which of the lenses makes it easier to see the chart or image. This vision test is not done with very young children or people who have trouble communicating.
What are visual field tests?
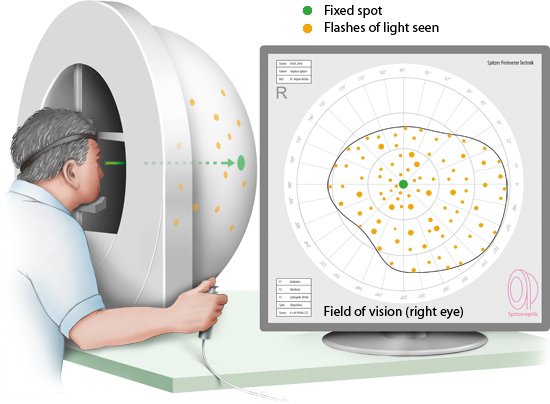
Your field of vision (or visual field) is what you are able to see without moving your eye. It can be tested using a bowl-shaped instrument known as a perimeter, so these tests are also known as perimetry tests.
With your head supported by a chin rest, you focus on a fixed spot at the center of the bowl. Moving flashes of light of varying degrees of brightness appear in different places inside the bowl. If you see a flash of light, you press a button. This makes it possible to measure the borders of the areas in which you can perceive something. The more areas in your field of vision are tested, the more accurate the test is – but it will then take longer as a result. Although perimetry tests aren't painful, they can be quite tiring because you have to concentrate for a long time.
Your field of vision is very important as it helps you know what is around you. It may be affected by damage to the retina or optic nerve, which can result from glaucoma or age-related macular degeneration (AMD). Neurological diseases like a stroke can also change your field of vision. So your field of vision is also checked if you have symptoms like unexplained headaches or dizziness.
How else can your vision be tested?
Vision is often assessed using other tests too. These include color vision tests, where you are asked to identify letters or numbers in multicolored pictures.
Your eye movement can be tested as well. That involves following a moving object with your eyes while holding your head still. The doctor can check the position of your eyes to each other by covering one eye and observing how the other one moves. This test is important in the diagnosis of squint in children, for example.
Your pupillary response (how your pupils react) can also be tested. A bright light is shone into your eyes. The pupils then reflexively react by narrowing.
What are slit-lamp examinations?
A slit lamp allows the doctor to examine your eye under magnification. As its name suggests, the lamp projects a narrow, slit-shaped beam of light into the eye.
It is easy to get a detailed view of the front part of the eye in particular by using a slit lamp, for example the different layers if the cornea. With an additional magnifying lens, the doctor can see into the back of the eye, such as the retina. Modern slit lamps also include a device that measures intraocular pressure.
You can use a chin rest for this examination as well. The doctor sits across from you and can examine one eye at a time.
What is ophthalmoscopy?
A special instrument known as an ophthalmoscope can be used to look at the fundus (back) of the eye through the pupil and examine structures like the retina, optic nerve, blood vessels and the choroid coat. This examination is known as ophthalmoscopy or funduscopy. About 20 minutes before the examination, the pupils of the eyes are dilated (enlarged) using eye drops.
In the direct exam, the doctor positions the ophthalmoscope close to the eye and shines a beam of light directly into it to see a small magnified section of the back of the eye. This is particularly useful for examining the structures at the center of the eye's fundus, including the optic nerve, the blood vessels and the macula.
In the indirect exam, the doctor uses a condensing lens with a bright light to examine the eye from a distance of about 60 centimeters. This allows them to see a larger area of the fundus, providing a better overview as well as a three-dimensional image. A slit lamp is sometimes used at the same time. Doing so greatly magnifies the retina and provides better lighting. To do this, the doctor holds the magnifying lens on the slit lamp or puts a contact glass directly on the eye. The eyes are numbed beforehand with eyed drops.
Conditions such as retinal detachment and optic nerve damage can be diagnosed using ophthalmoscopy. It can also be a good idea to examine the small blood vessels in your eye if you have diabetes or high blood pressure.
How is intraocular pressure measured?
Intraocular pressure is often measured by eye doctors. The medical term for this examination is tonometry.
Your eye is constantly producing more of a fluid called aqueous humor. Among other things, it supplies nutrients to the lens and the cornea, and it prevents the growth of bacteria. The intraocular pressure regulates the balance between the newly produced aqueous humor and the “old” aqueous humor. The pressure increases if the aqueous humor can't drain properly and starts to build up. An intraocular pressure of between 10 and 21 mmHg (millimeters of mercury) is considered to be normal in adults.
There are various ways to measure the pressure in the eye: In what is known as applanation tonometry, the cornea is first numbed using eye drops. Then a small sensor about three millimeters in diameter is placed in the middle of the cornea and pressed lightly against the eye. The device measures how much pressure is needed to flatten the cornea under it. This is a measure of the pressure inside the eye.
Intraocular pressure can also be measured using an approach known as non-contact tonometry. Here the pressure is measured by applying a short puff of air to the cornea. Neither of these tests are painful.
What other kinds of eye examinations are there?
Other eye examinations can be done to confirm certain diagnoses and help plan treatment.
For instance, the retina can be examined using fluorescein angiography. This involves injecting a fluorescent dye into a vein in the arm. The dye spreads through all the blood vessels in the body, including those in the retina. The doctor can then use a special camera to detect changes in the blood vessels of the eye.
Optical coherence tomography (OCT) is another type of eye examination. OCT uses a laser to measure things like the thickness of the retina. This technique can be applied to detect the build-up of fluid in the retina.
Various ultrasound tests can also be used to examine the eye: The transducer is often placed on your closed eyelid. Sometimes it’s necessary to place it directly on your eye. Then, eye drops are used to numb your eye first. Ultrasound can be used to measure the length of your eyeball. This may be done before surgery on the lens of your eye to treat nearsightedness or cataracts. It is also possible to detect thickening of eye muscles, circulation problems, or tumors using ultrasound.
Andreae S, Avelini P, Berg M et al. Lexikon der Krankheiten und Untersuchungen. Stuttgart: Thieme; 2008.
Berufsverband der Augenärzte Deutschlands (BVA), Deutsche Ophthalmologische Gesellschaft (DOG). Augenärzliche Basisdiagnostik bei Patienten ab dem 7. Lebensjahr (Leitlinie Nr. 4). 1998.
Dahlmann C, Patzelt J. Basics Augenheilkunde. Munich: Urban und Fischer; 2020.
Grehn F. Augenheilkunde. Stuttgart: Thieme; 2019.
Lang GK, Lang SJ. Augenheilkunde. Stuttgart: Thieme; 2024.
Pschyrembel Online. 2024.
IQWiG health information is written with the aim of helping people understand the advantages and disadvantages of the main treatment options and health care services.
Because IQWiG is a German institute, some of the information provided here is specific to the German health care system. The suitability of any of the described options in an individual case can be determined by talking to a doctor. informedhealth.org can provide support for talks with doctors and other medical professionals, but cannot replace them. We do not offer individual consultations.
Our information is based on the results of good-quality studies. It is written by a team of health care professionals, scientists and editors, and reviewed by external experts. You can find a detailed description of how our health information is produced and updated in our methods.
Stay informed
Subscribe to our newsletter or newsfeed. You can find our growing collection of films on YouTube.