Introduction

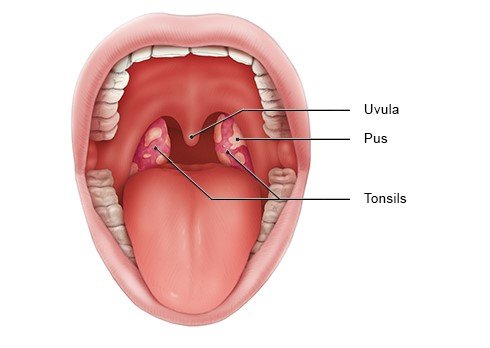
Sore throats can have a range of causes. They usually result from an inflammation of the throat caused by cold viruses. This can also affect the palatine tonsils. Often simply referred to as "tonsils," these are the visible lumps of tissue on the left and right sides at the back of the throat. Bacterial infections of the tonsils are less common. But it isn’t easy to tell what kind of germs are responsible for the infection. Children and teenagers are much more susceptible to tonsillitis ( inflammation of the tonsils) than adults are.
Tonsillitis starts suddenly and is painful, but it usually goes away within one to two weeks. But it may also return several times. Although that can be unpleasant, it only rarely results in complications.
It is important to distinguish between tonsillitis and enlarged tonsils. These are two separate medical conditions. In enlarged tonsils, the adenoids may be affected as well.