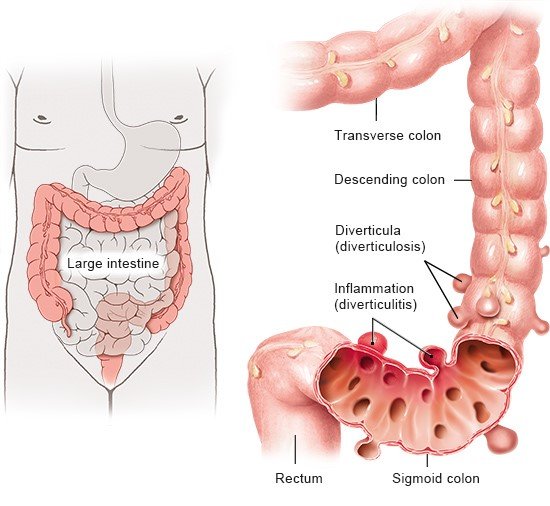
Diverticula often remain unnoticed if they don’t cause any symptoms. But they sometimes lead to chronic digestive problems and pain, or may even become inflamed or infected.
Diverticulitis can usually be treated effectively and then goes away after a few weeks. But about 20% of those affected get diverticulitis again within a few years.
Diverticulitis can lead to complications if the inflammation spreads to the wall of the intestine, surrounding tissue or nearby organs. Abscesses (collections of pus) or fistulas may develop. A fistula is an abnormal tunnel-like passageway between two organs, for instance between the intestine and the bladder.
One rare but serious complication may arise if the wall of the intestine tears (intestinal perforation). If the contents of the intestine then leak out into the abdominal cavity, the inner lining of the tummy (peritoneum) may become inflamed, leading to a life-threatening condition known as peritonitis. This typically causes severe tummy pain, a hard abdominal wall, fever, nausea, a rapid heartbeat and general weakness. If symptoms like this occur, it's important to see a doctor right away.
In some people, diverticula keep becoming inflamed despite having been treated successfully in the past. This can lead to scarring that causes the intestine to become narrow (stenosis), making it difficult for stool to pass through it. In extreme cases, the intestine becomes blocked (ileus). Some people have constant symptoms although their intestine isn’t inflamed. The risk of complications is greatest when someone has diverticulitis for the first time. After that, recurring inflammations are a lot less likely to lead to complications. The main consequences of recurring diverticulitis are chronic symptoms such as irregular bowel movements, bloating and abdominal pain.
It is good to know that diverticula do not develop into bowel cancer. This kind of cancer develops from polyps in the bowel.