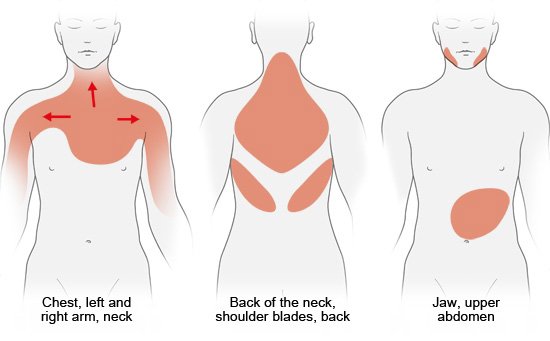
Symptoms in the chest area can be caused by many different things, including problems affecting the muscles or bones in the rib cage. Diseases of the lungs, food pipe or the airways can also cause chest pains, as can emotional strain and mental illnesses. Other cardiovascular diseases such as heart muscle inflammations (myocarditis) and irregular heartbeats can also cause similar symptoms.
To get an idea of whether it's CAD, the doctor will first ask your age, whether you have any other diseases, what exactly the symptoms feel like and when they occur. They will also ask about cardiovascular disease in your family and about risk factors such as smoking. They will do a physical examination of your chest, too.
If the doctor suspects you have CAD, the most important examination is an electrocardiogram (ECG). This is done either while you're resting or while you're exercising. It is also possible to do an ultrasound scan of the heart (echocardiography) or use another imaging technique to examine the heart. Whether further heart tests are needed, and what kind, will depend on your age, any other medical conditions you have, and your symptoms.
To assess the risk of complications and make a treatment plan, your doctor will suggest having several other tests. The diagnosis typically involves:
- Measuring blood pressure: Blood pressure is measured because if someone who has CAD also has high blood pressure, the CAD is more likely to lead to complications.
- Physical examinations: Examinations such as listening to the heart or feeling the liver can help to find out whether you might have other conditions such as heart failure or heart valve problems.
- Test for metabolic disorders: A blood sample is usually taken as well, to look for any metabolic disorders such as type 2 diabetes or to measure your cholesterol level. Type 2 diabetes can greatly increase the risk of developing complications.
In the long term, it's a good idea to have regular check-ups with your family doctor to keep an eye on how the CAD develops, adjust treatment, and discuss your personal goals and any problems. Check-ups every 3 to 6 months are recommended.