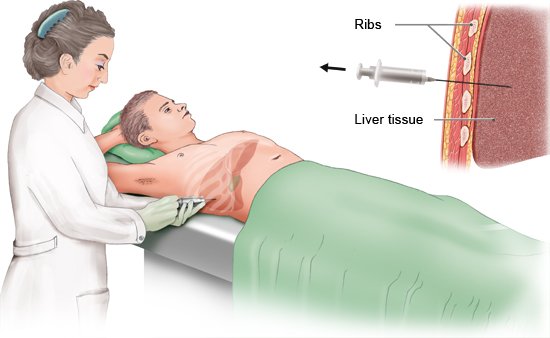
What happens during a biopsy?
A biopsy (taking a tissue sample) is one of the most commonly used medical examinations. Tissue samples can be analyzed in order to find out, for instance, whether a suspicious lump is harmless or dangerous. The doctor removes a small sample of tissue and sends it to a laboratory to be examined under a microscope. The tissue sample can often be removed in an outpatient setting (without an overnight stay).