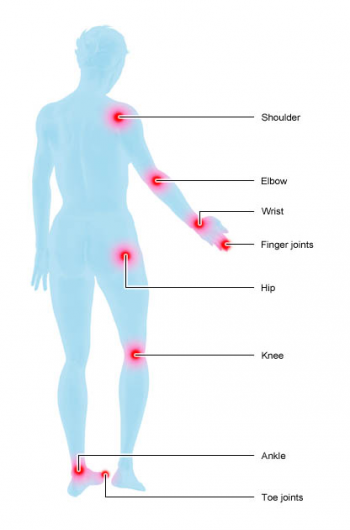
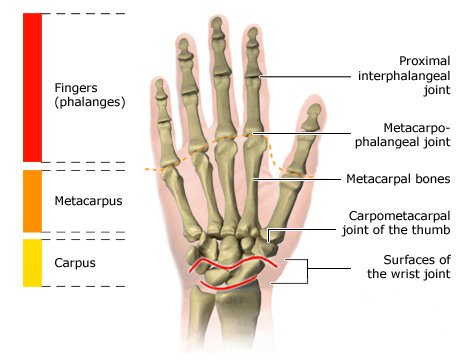
Rheumatoid arthritis can be treated with medication, physical therapy and occupational therapy. There are also various support aids that can make some everyday tasks easier. People are advised to do regular exercise or sports too.
The treatment options will depend on things like
- how severe the inflammation and symptoms are,
- how far the disease has progressed,
- the predicted further course of the disease, and
- how well previous treatments have worked.
There is currently no cure for rheumatoid arthritis. But medication can
- reduce inflammation,
- stop the disease from getting worse,
- relieve symptoms like pain and swelling, and
- help people move their joints more easily again or maintain joint mobility for as long as possible.
Physical therapy and sports can help improve or maintain mobility, strength and joint function. Examples of suitable types of sports include cycling, brisk walking, dancing, doing exercises (e.g. gentle strengthening exercises), swimming and aqua aerobics.
The main aim of occupational therapy is to maintain your mobility and hand strength, and to learn how to get by with rheumatoid arthritis in daily life.
Psychological treatments can help relieve pain and minimize the impact it has on everyday life. They are also supposed to help relieve disease-related anxiety and depression that some people develop.
If medication is not able to relieve the symptoms and the arthritis keeps getting worse, the thin layer that lines the joint (synovium) can be surgically removed. Surgery can reduce the pain and symptoms caused by severe joint damage resulting from rheumatoid arthritis. That may involve implanting an artificial joint or fusing the joint (arthrodesis), for example.
In advanced arthritis, various aids can compensate for many physical limitations and help you to carry out everyday activities. These include orthopedic shoe inserts, grabbing aids and specially designed cutlery.