Topical medications (applied to the skin)
Steroid ointments, creams and lotions can be very effective in treating skin rashes. This means that they're especially useful in the treatment of inflammatory skin conditions such as psoriasis or any type of eczema. But for many other skin conditions they are ineffective or even harmful. Acne, rosacea and infectious diseases such as a fungal skin infection can even be made worse by steroid medications. So it's important to have an exact diagnosis before using steroids.
Possible side effects
The possible side effects of topical treatment with steroids are inflammations of the hair follicles, mild pigmentation disorders on the skin (white spots) and stretch marks. Many people are especially concerned about their skin getting thinner. If that happens, small, widened blood vessels under the skin that look like spiderwebs become visible (this is known as spider veins or teleangiectasia). But if topical steroids are used properly, the risk of these and other side effects is very small. And if the skin starts to change and the treatment is stopped, the skin can then recover.
Safe use
In order to avoid side effects, the strength of the steroid medication has to be suitable for the thickness and sensitivity of the skin area to be treated.
Not all steroids are the same: There are more than 30 different glucocorticoid drugs of varying strength (potency). They are divided into four groups:
- Low-potency topical steroids, e.g. hydrocortisone and prednisolone
- Medium-potency topical steroids like prednicarbate, methylprednisolone aceponate
- High-potency topical steroids such as betamethasone valerate and mometasone furoate
- Ultra-high-potency topical steroids, such as clobetasol propionate
Steroids are more potent where the skin is thin and sensitive, particularly on
- the face,
- the inner sides of joints, such as the back of the knee, the insides of the elbows and upper arms, and the armpits, as well as
- the eyelids and genitals.
Low-potency or medium-potency medication is usually enough for treating the face and the skin on the inner sides of the joints. Eyelids and genitals should only be treated with low-potency medication. Higher-potency medication is often needed to treat the scalp and the hands and feet. The skin in these areas is relatively thick, so only small amounts of the medicine can reach the deeper layers of skin. But the risk of the skin thinning on these parts of the body is very low, even if high-potency medication is applied.
Besides the potency of the medication and the thickness of the skin, the effects of a steroid medication depend on the following factors:
- The dose
- The type of product: Steroid ointments are a little stronger than steroid creams or lotions. This is because steroids are more easily absorbed by the skin when applied as an ointment.
- How it is applied: Topical steroids have a stronger effect when applied to wet skin – for instance after taking a bath – than when applied to dry skin. If you also cover the area of skin with a bandage or a wet wrap, it will absorb much more of the drug. It is especially important to keep this in mind with young children if the treated area of their skin is covered by a diaper (nappy).
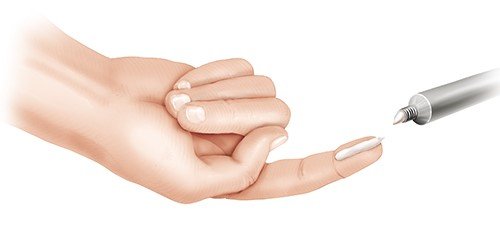
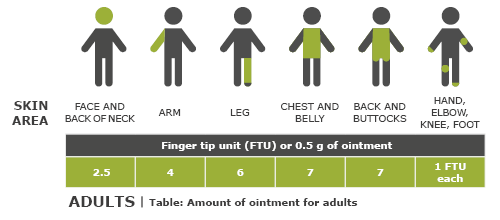
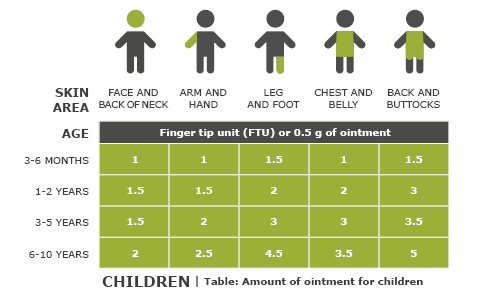
Many people who use steroid medications on their skin tend to apply either too much or too little, usually because they’re not sure how to apply them correctly or because they’re afraid of the side effects. You can use the fingertip unit (FTU) to get an idea of how much to use: One FTU is the amount of ointment that fits on the last section of an adult's finger (see illustration). This is about 0.5 grams. One half of a FTU is enough to apply to an area of skin the size of the palm of one hand plus the insides of the fingers.